Call Us: (239) 427-1455
This site is for families seeking memory care services. For employment inquiries, visit our Indeed page.
Redefining Memory Care In Estero Florida
Choosing the right memory care community for a loved one is a deeply personal decision. At Gulf Coast Memory Care, conveniently located next to Coconut Point Shopping Center in Estero, Florida, we've created a haven of tranquility where residents can experience a luxurious and comfortable lifestyle. Let us help you make this important decision with confidence.
"Choose us with peace of mind; if within 90 days your heart pulls you elsewhere, we'll ensure a smooth transition and give your community fee back to help secure another place."
Your family's freedom to thrive is our top priority.

Award Winning Leadership

Understanding The Benefits Of Memory Care
Hear From Jen
We believe that exceptional care begins with open, honest, and ongoing communication. Families have direct access to our leadership and caregivers, including personal cell numbers, because staying informed should never be a struggle.
Every resident also receives a personalized care plan tailored to their needs, so families always stay connected.
Is It The Right Time For Memory Care?
Understanding that memory care is not a one-size-fits-all solution, we prioritize personalized care plans that adapt to each individual’s progression.
Learn more about senior care and get personalized results in this quick 5 minute survey.


A Community For Alzheimer’s & Dementia Care
Families seeking Alzheimer’s and dementia support in Estero, Florida, can rely on our compassionate team for a community that truly cares.
Through ongoing training in the latest memory care practices and a commitment to safety, Gulf Coast Memory Care offers peace of mind for families and the highest standard of care for residents.
Love From Our Families


My mom moved into her new home a few weeks ago. I was able to visit with her this week while being in Florida and my gosh, I know she is right where she needs to be. Huge shoutout to Jerry, Diana, Paula, Kathy and Apryl. You are real life angels. The energy you bring is above and beyond. To see how you interact with not only my mom, but all the residents, it truly warms my heart. While it is heartbreaking to see my mom battle Alzheimer's, I know she is in the perfect place. She is safe and receiving the care she needs. <3 The place is clean, accommodating and most importantly feels like home. I love that there is a schedule and many activities for the residents to participate in. My mom has loved the painting and coloring
- Bill & Bonny B

Shelly Richardson

Upon entering this beautiful community, I was deeply impressed by the exceptional level of care and compassion demonstrated by all the caregivers. Every member of the team, from maintenance staff to the executive director, significantly contributes to the residents' quality of life. The interior courtyards offer a safe and beautiful outdoor escape for the residents, while the dining area is both elegant and spacious. GCMC stands out as one of the premier memory care centers I have ever visited.
- Bill & Bonny B


Exceptional dedication. Genuine care 24/7, everyone is doing a great job, from Management to the care team. Jerry and Diana are conducting the business, but you can see them walking the hallway and chatting with the residents, literally knowing everyone. There is an engine who works behind the scenes to have the day and night activity running smoothly. Family feeling, warmth, and genuine care, overall, 5 stars. Residents are never alone, there is always a pair of eyes to watch and hands ready to help as needed, but all is done in a certain way, so our loved ones don’t feel any loss of their independence. Beautifully done. The activities are not just lines on paper, everyone is involved. Food is first class.
- Bill & Bonny B
Our Senior Care Amenities

One-site beauty salon and barbershop
Personalized, chef-prepared meals
Customized activity programs
Craft and hobby room
Family living room
Full Library
Abundant natural light to minimize sundowning
Located next to Coconut Point Shopping Center
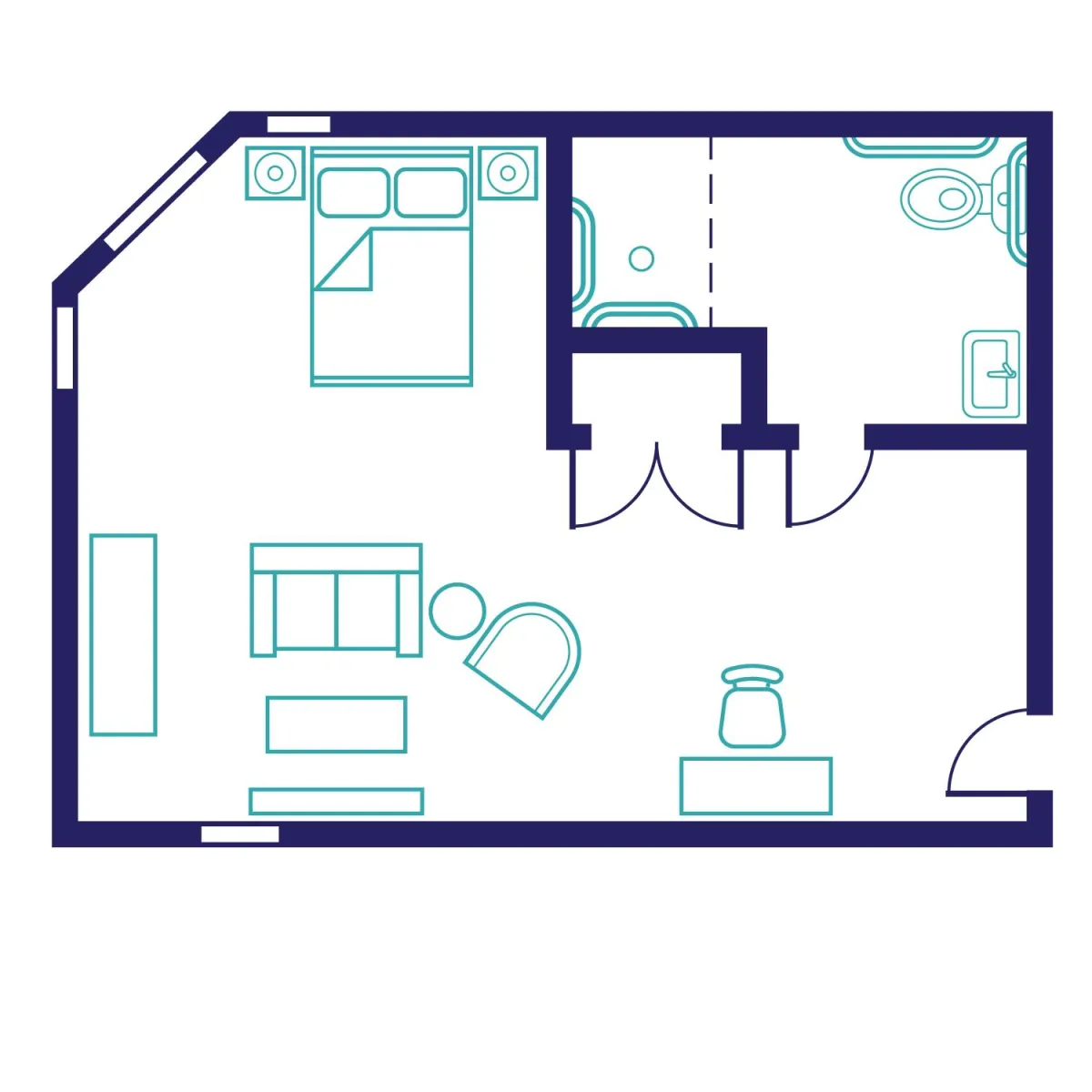
The Edison Suite
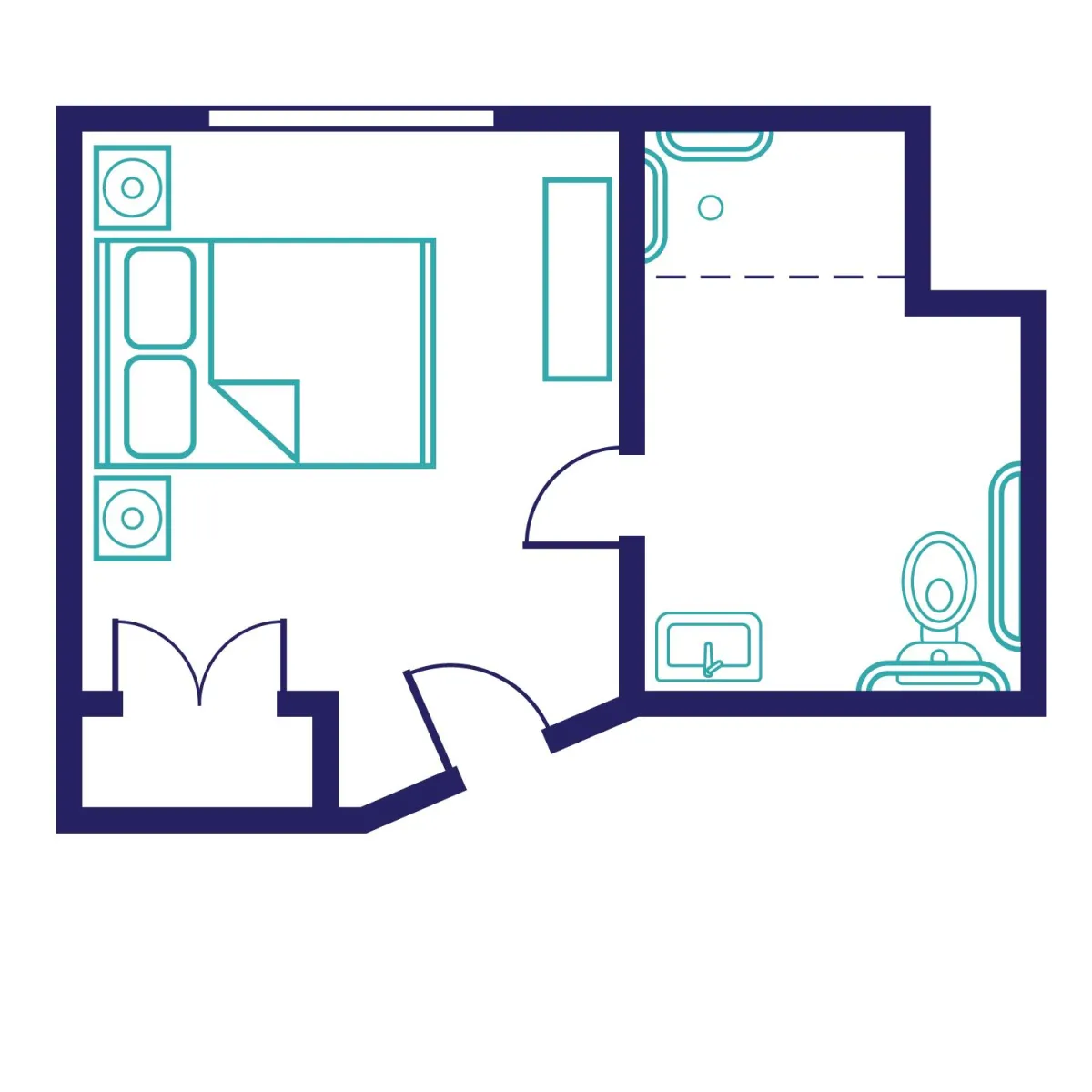
The Magnolia Suite
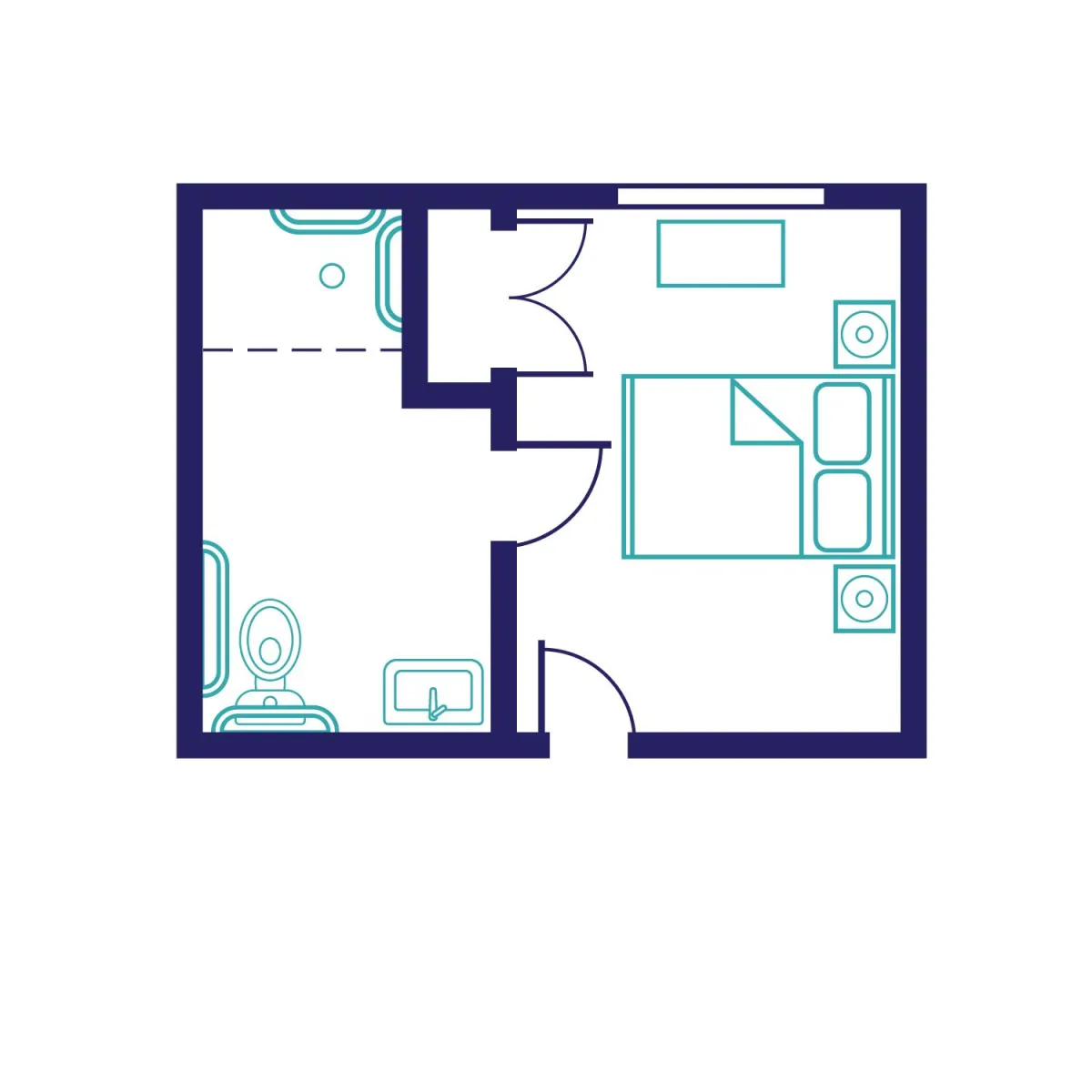
The Sugarberry Suite

Engaging Residents With Meaningful Social Connections
We also prioritize activities that nurture both physical and mental wellness, from gentle exercise routines to social events that create a sense of community among residents. These carefully crafted programs are designed to boost mood, reduce anxiety, and encourage meaningful interactions, all of which contribute to a fulfilling lifestyle for those facing memory challenges.
Our Commitment To You
Our commitment extends to providing families with guidance and resources to understand memory loss and navigate the journey with confidence. Whether it’s through educational workshops or one-on-one consultations, we’re here to support families every step of the way, ensuring they feel connected and informed about their loved one’s care journey.


Are You Ready To Get Settled In?
Embark on a transformative experience at Gulf Coast Memory Care in Estero, Florida. We're not just a memory care community; we're a sanctuary where the mind, body, and spirit are nurtured. If you're seeking a place where compassion, care, and a deep respect for the human soul are paramount, you've found the right haven.
Check Out Our Blog

Understanding Personality Changes in Dementia: Why Your Loved One Seems Different
One of the most heartbreaking aspects of dementia isn't just memory loss—it's when your loved one's personality seems to change. The gentle parent becomes aggressive. The social butterfly withdraws. The patient spouse becomes irritable. At Gulf Coast Memory Care, families often ask: "Is this still my loved one?" Understanding why personality changes happen can help you navigate this difficult reality with compassion and realistic expectations.
Why Dementia Changes Personality
The Brain Science Behind Behavioral Shifts
Personality changes in dementia aren't about choice or willpower—they're neurological. Dementia damages specific brain regions that control:
Frontal Lobe (Executive Function):
Impulse control
Social judgment
Emotional regulation
Decision-making
Temporal Lobe (Emotional Processing):
Emotional responses
Recognition of social cues
Memory of relationships
Amygdala (Emotional Center):
Fear and anxiety responses
Emotional reactions
Aggression triggers
When these areas deteriorate, the person you knew may seem fundamentally different—not because they've chosen to change, but because their brain can no longer regulate personality the way it once did.
Common Personality Changes and What They Mean
From Outgoing to Withdrawn
What You See:
Avoiding social situations
Loss of interest in hobbies
Reduced conversation
Preferring isolation
What's Happening:
Difficulty processing social interactions
Anxiety about confusion or mistakes
Exhaustion from cognitive effort
Loss of confidence
How GCMC Helps: Our Rhythm of Life programming provides structured social opportunities that reduce anxiety while encouraging gentle engagement. Activities are designed for all dementia stages, with staff support to help residents participate comfortably.
From Calm to Agitated
What You See:
Increased irritability
Angry outbursts
Restlessness or pacing
Resistance to care
What's Happening:
Inability to express needs verbally
Frustration with cognitive decline
Sensory overload
Unmet physical or emotional needs
How GCMC Helps: Our staff receives specialized training in Teepa Snow methods and de-escalation techniques. With an 8:1 staff-to-resident ratio, team members can identify triggers early and respond with personalized comfort strategies.
The Alzheimer's Association provides additional guidance on managing behavioral changes.
From Trusting to Suspicious
What You See:
Accusations of theft
Paranoia about caregivers
Distrust of family members
Hiding belongings
What's Happening:
Memory loss creates confusion about missing items
Difficulty recognizing familiar people
Brain damage affecting judgment centers
Fear response to confusion
How GCMC Helps: Consistent caregivers build trust over time. Our team understands that suspicion isn't personal—it's a symptom. We use validation techniques rather than arguing or correcting.
From Reserved to Inappropriate
What You See:
Sexually inappropriate comments or behavior
Loss of social filters
Saying hurtful things
Public undressing
What's Happening:
Frontal lobe damage removes inhibitions
Confusion about appropriate behavior
Misinterpretation of physical sensations
Loss of social awareness
How GCMC Helps: Our trained staff responds with dignity-preserving redirection. We understand these behaviors are neurological, not intentional, and we protect resident privacy while addressing needs compassionately.
From Independent to Clingy
What You See:
Following caregivers constantly
Anxiety when alone
Repeated questions about your whereabouts
Distress at separation
What's Happening:
Loss of sense of time and permanence
Anxiety from confusion
Fear of abandonment
Need for security and reassurance
How GCMC Helps: Consistent routines and familiar faces provide security. Our 24/7 care means residents always have supportive staff nearby, reducing anxiety about being alone.
What Families Need to Know
It's Not Personal (Even When It Feels That Way)
When Your Loved One:
Doesn't recognize you
Says hurtful things
Prefers staff over family
Accuses you of abandonment
Remember:
The disease is speaking, not your loved one
Brain damage affects recognition and judgment
Emotional responses are neurological
Your relationship's history still matters, even if they can't express it
Some Core Essence Often Remains
What May Stay:
Emotional responses to music they loved
Comfort from familiar routines
Reactions to kindness and gentleness
Moments of connection and joy
What Changes:
How they express themselves
Ability to control impulses
Social awareness
Emotional regulation
Supporting Your Loved One Through Personality Changes
Validation Over Correction
Instead of: "No, I didn't steal your purse. You're in memory care."
Try: "That must be frustrating. Let's look for it together."
Instead of: "Stop being so mean. That's not like you."
Try: "I can see you're upset. How can I help?"
Instead of: "You just asked me that five minutes ago."
Try: Answer again as if it's the first time.
Environmental Modifications
Reduce Triggers:
Minimize noise and overstimulation
Maintain consistent routines
Use calming sensory experiences
Ensure physical comfort (pain, hunger, bathroom needs)
GCMC's Approach:
Abundant natural light reduces agitation
Interior courtyards provide calming outdoor access
Consistent daily schedules through Rhythm of Life
Personalized care plans address individual triggers
Medication Considerations
When to Discuss with Medical Team:
Personality changes causing distress or danger
Aggressive behaviors affecting care
Severe anxiety or depression
Sleep disturbances
GCMC's Role: We monitor behavioral patterns and communicate changes to families and medical partners. Medication is never a first response—we prioritize behavioral interventions and environmental modifications.
Frequently Asked Questions
Q: Will my loved one's personality keep changing? A: Yes, as dementia progresses, personality changes often continue. Each stage may bring new challenges and adjustments.
Q: Can anything reverse personality changes? A: No, but proper care, medication management, and environmental support can reduce distressing behaviors and improve quality of life.
Q: How do I explain personality changes to other family members? A: Share educational resources about dementia's neurological effects. Help them understand these changes are symptoms, not choices.
Q: Should I correct inappropriate behavior? A: Gentle redirection works better than correction. Focus on dignity and comfort rather than teaching or disciplining.
Q: What if I don't like who my loved one has become? A: This grief is valid and common. Seek support through counseling, support groups, or talking with GCMC staff who understand.
Grieving the Person They Were
Ambiguous Loss
What It Means: Your loved one is physically present but psychologically changed. This creates a unique grief—mourning someone who's still alive.
It's Normal to Feel:
Sadness for the relationship lost
Anger at the disease
Guilt about negative feelings
Relief when care becomes professional
Love mixed with frustration
Finding Support:
Family caregiver support groups
Counseling specializing in dementia grief
Connection with other families at GCMC
Staff who understand and validate your experience
Related Resource: Learn about family caregiver support → here.
The Family Caregiver Alliance offers resources for coping with dementia-related grief.
How GCMC Supports Residents Through Personality Changes
Individualized Care Plans
We Consider:
Life history and personality before dementia
Current behavioral patterns and triggers
Successful comfort strategies
Family input and preferences
Staff Training and Consistency
Our Team Receives:
Teepa Snow dementia communication training
De-escalation and behavior management techniques
Understanding of neurological causes
Compassionate response strategies
Why Consistency Matters: Familiar faces and consistent approaches reduce anxiety and build trust, even as personality changes progress.
Hear from Rachel about her experience navigating personality changes in her loved one and how Gulf Coast Memory Care's specialized approach made a difference in their family's journey.
24/7 Specialized Support
With our 8:1 staff-to-resident ratio, team members can:
Respond immediately to behavioral changes
Identify triggers and patterns
Provide personalized comfort
Communicate changes to families
Key Takeaways
✓ Personality changes are neurological, not intentional
✓ Dementia damages brain regions controlling behavior and emotion
✓ Validation works better than correction
✓ Some core essence often remains despite changes
✓ GCMC staff are trained in compassionate behavioral support
✓ Grief over personality changes is normal and valid
✓ Professional care provides specialized support families can't replicate at home
Moving Forward with Compassion
Understanding that personality changes are symptoms—not choices—doesn't make them less painful. But it can help you respond with compassion rather than frustration, and seek appropriate support rather than blame yourself or your loved one.
At Gulf Coast Memory Care, we see families navigate this heartbreaking reality every day. Our team understands that the person you're visiting isn't exactly who they used to be—and that's okay. We honor who they were while caring for who they are now.
The parent who raised you, the spouse who built a life with you—their essence deserves respect and dignity, even when dementia changes how they express themselves. That's the foundation of everything we do.
Struggling with personality changes in your loved one? Contact Gulf Coast Memory Care to learn how our specialized training, consistent care approach, and compassionate team support residents and families through behavioral challenges. Schedule a tour to see our dementia-focused care in action.
Call Us: (239) 427-1455

Understanding Personality Changes in Dementia: Why Your Loved One Seems Different
One of the most heartbreaking aspects of dementia isn't just memory loss—it's when your loved one's personality seems to change. The gentle parent becomes aggressive. The social butterfly withdraws. The patient spouse becomes irritable. At Gulf Coast Memory Care, families often ask: "Is this still my loved one?" Understanding why personality changes happen can help you navigate this difficult reality with compassion and realistic expectations.
Why Dementia Changes Personality
The Brain Science Behind Behavioral Shifts
Personality changes in dementia aren't about choice or willpower—they're neurological. Dementia damages specific brain regions that control:
Frontal Lobe (Executive Function):
Impulse control
Social judgment
Emotional regulation
Decision-making
Temporal Lobe (Emotional Processing):
Emotional responses
Recognition of social cues
Memory of relationships
Amygdala (Emotional Center):
Fear and anxiety responses
Emotional reactions
Aggression triggers
When these areas deteriorate, the person you knew may seem fundamentally different—not because they've chosen to change, but because their brain can no longer regulate personality the way it once did.
Common Personality Changes and What They Mean
From Outgoing to Withdrawn
What You See:
Avoiding social situations
Loss of interest in hobbies
Reduced conversation
Preferring isolation
What's Happening:
Difficulty processing social interactions
Anxiety about confusion or mistakes
Exhaustion from cognitive effort
Loss of confidence
How GCMC Helps: Our Rhythm of Life programming provides structured social opportunities that reduce anxiety while encouraging gentle engagement. Activities are designed for all dementia stages, with staff support to help residents participate comfortably.
From Calm to Agitated
What You See:
Increased irritability
Angry outbursts
Restlessness or pacing
Resistance to care
What's Happening:
Inability to express needs verbally
Frustration with cognitive decline
Sensory overload
Unmet physical or emotional needs
How GCMC Helps: Our staff receives specialized training in Teepa Snow methods and de-escalation techniques. With an 8:1 staff-to-resident ratio, team members can identify triggers early and respond with personalized comfort strategies.
The Alzheimer's Association provides additional guidance on managing behavioral changes.
From Trusting to Suspicious
What You See:
Accusations of theft
Paranoia about caregivers
Distrust of family members
Hiding belongings
What's Happening:
Memory loss creates confusion about missing items
Difficulty recognizing familiar people
Brain damage affecting judgment centers
Fear response to confusion
How GCMC Helps: Consistent caregivers build trust over time. Our team understands that suspicion isn't personal—it's a symptom. We use validation techniques rather than arguing or correcting.
From Reserved to Inappropriate
What You See:
Sexually inappropriate comments or behavior
Loss of social filters
Saying hurtful things
Public undressing
What's Happening:
Frontal lobe damage removes inhibitions
Confusion about appropriate behavior
Misinterpretation of physical sensations
Loss of social awareness
How GCMC Helps: Our trained staff responds with dignity-preserving redirection. We understand these behaviors are neurological, not intentional, and we protect resident privacy while addressing needs compassionately.
From Independent to Clingy
What You See:
Following caregivers constantly
Anxiety when alone
Repeated questions about your whereabouts
Distress at separation
What's Happening:
Loss of sense of time and permanence
Anxiety from confusion
Fear of abandonment
Need for security and reassurance
How GCMC Helps: Consistent routines and familiar faces provide security. Our 24/7 care means residents always have supportive staff nearby, reducing anxiety about being alone.
What Families Need to Know
It's Not Personal (Even When It Feels That Way)
When Your Loved One:
Doesn't recognize you
Says hurtful things
Prefers staff over family
Accuses you of abandonment
Remember:
The disease is speaking, not your loved one
Brain damage affects recognition and judgment
Emotional responses are neurological
Your relationship's history still matters, even if they can't express it
Some Core Essence Often Remains
What May Stay:
Emotional responses to music they loved
Comfort from familiar routines
Reactions to kindness and gentleness
Moments of connection and joy
What Changes:
How they express themselves
Ability to control impulses
Social awareness
Emotional regulation
Supporting Your Loved One Through Personality Changes
Validation Over Correction
Instead of: "No, I didn't steal your purse. You're in memory care."
Try: "That must be frustrating. Let's look for it together."
Instead of: "Stop being so mean. That's not like you."
Try: "I can see you're upset. How can I help?"
Instead of: "You just asked me that five minutes ago."
Try: Answer again as if it's the first time.
Environmental Modifications
Reduce Triggers:
Minimize noise and overstimulation
Maintain consistent routines
Use calming sensory experiences
Ensure physical comfort (pain, hunger, bathroom needs)
GCMC's Approach:
Abundant natural light reduces agitation
Interior courtyards provide calming outdoor access
Consistent daily schedules through Rhythm of Life
Personalized care plans address individual triggers
Medication Considerations
When to Discuss with Medical Team:
Personality changes causing distress or danger
Aggressive behaviors affecting care
Severe anxiety or depression
Sleep disturbances
GCMC's Role: We monitor behavioral patterns and communicate changes to families and medical partners. Medication is never a first response—we prioritize behavioral interventions and environmental modifications.
Frequently Asked Questions
Q: Will my loved one's personality keep changing? A: Yes, as dementia progresses, personality changes often continue. Each stage may bring new challenges and adjustments.
Q: Can anything reverse personality changes? A: No, but proper care, medication management, and environmental support can reduce distressing behaviors and improve quality of life.
Q: How do I explain personality changes to other family members? A: Share educational resources about dementia's neurological effects. Help them understand these changes are symptoms, not choices.
Q: Should I correct inappropriate behavior? A: Gentle redirection works better than correction. Focus on dignity and comfort rather than teaching or disciplining.
Q: What if I don't like who my loved one has become? A: This grief is valid and common. Seek support through counseling, support groups, or talking with GCMC staff who understand.
Grieving the Person They Were
Ambiguous Loss
What It Means: Your loved one is physically present but psychologically changed. This creates a unique grief—mourning someone who's still alive.
It's Normal to Feel:
Sadness for the relationship lost
Anger at the disease
Guilt about negative feelings
Relief when care becomes professional
Love mixed with frustration
Finding Support:
Family caregiver support groups
Counseling specializing in dementia grief
Connection with other families at GCMC
Staff who understand and validate your experience
Related Resource: Learn about family caregiver support → here.
The Family Caregiver Alliance offers resources for coping with dementia-related grief.
How GCMC Supports Residents Through Personality Changes
Individualized Care Plans
We Consider:
Life history and personality before dementia
Current behavioral patterns and triggers
Successful comfort strategies
Family input and preferences
Staff Training and Consistency
Our Team Receives:
Teepa Snow dementia communication training
De-escalation and behavior management techniques
Understanding of neurological causes
Compassionate response strategies
Why Consistency Matters: Familiar faces and consistent approaches reduce anxiety and build trust, even as personality changes progress.
Hear from Rachel about her experience navigating personality changes in her loved one and how Gulf Coast Memory Care's specialized approach made a difference in their family's journey.
24/7 Specialized Support
With our 8:1 staff-to-resident ratio, team members can:
Respond immediately to behavioral changes
Identify triggers and patterns
Provide personalized comfort
Communicate changes to families
Key Takeaways
✓ Personality changes are neurological, not intentional
✓ Dementia damages brain regions controlling behavior and emotion
✓ Validation works better than correction
✓ Some core essence often remains despite changes
✓ GCMC staff are trained in compassionate behavioral support
✓ Grief over personality changes is normal and valid
✓ Professional care provides specialized support families can't replicate at home
Moving Forward with Compassion
Understanding that personality changes are symptoms—not choices—doesn't make them less painful. But it can help you respond with compassion rather than frustration, and seek appropriate support rather than blame yourself or your loved one.
At Gulf Coast Memory Care, we see families navigate this heartbreaking reality every day. Our team understands that the person you're visiting isn't exactly who they used to be—and that's okay. We honor who they were while caring for who they are now.
The parent who raised you, the spouse who built a life with you—their essence deserves respect and dignity, even when dementia changes how they express themselves. That's the foundation of everything we do.
Struggling with personality changes in your loved one? Contact Gulf Coast Memory Care to learn how our specialized training, consistent care approach, and compassionate team support residents and families through behavioral challenges. Schedule a tour to see our dementia-focused care in action.
Call Us: (239) 427-1455
Come Visit Us
We can't wait to hear from you! Fill out our contact form to get started or if you would like to see our community for yourself, schedule a tour here.
Gulf Coast Memory Care
(239) 427-1455
22900 Lyden Dr, Estero, FL 33928
AL# 12921
Privacy Policy | Accessibility Statement | Visitation Policy